
Company:Acacium Group (digital health consultancy partnering with the NHS to deliver health platforms)
Role:UX Researcher and Designer
Project duration:2 months
Design team size:2 Designers
Skills:Research, stakeholder interviews, journey mapping, agile UX, usability testing,
recommendations for stakeholders
Output & impact:Digital health platform delivered
Summary/Context
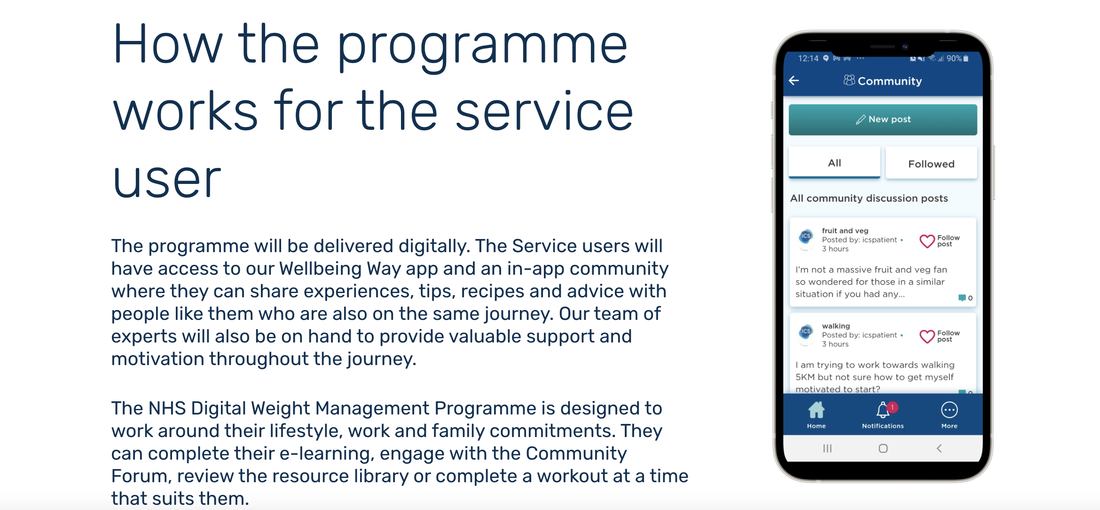
During the COVID-19 pandemic, Acacium Group developed a critical digital health solution for the NHS to support diabetic patients unable to attend in-person appointments. Traditional diabetes care had to transform into a comprehensive digital wellness platform to ensure continuity of care during healthcare disruption.The challenge was to design a telehealth platform that was accessible to diverse patient groups, secure for medical communication, engaging through community support, and compliant with NHS clinical standards — all during a national health crisis.
Project phases
Research questions
Research goals
Challenges
Approach
Deliverables & impact
Research questions
- How do diabetic patients manage their condition when in-person clinical support is unavailable?
- What are the critical touchpoints where digital intervention can provide the most impact?
- What barriers do diabetic patients face in adopting telehealth platforms?
- How can community support be integrated into a clinical platform without compromising medical credibility?
- What do healthcare providers need from a digital platform to deliver effective remote diabetes management?
Research goals
- Understand how diabetic patients' care needs changed during COVID-19 lockdown.
- Map the healthcare journey and identify where digital tools could replace or enhance in-person care.
- Define requirements for virtual consultations, tracking, and community features from both patient and provider perspectives.
- Document NHS clinical standards and compliance requirements.
- Validate design concepts with real patients to ensure accessibility across diverse user groups.
Challenges
Challenge: Pandemic lockdown prevented in-person research with vulnerable diabetic patients. Adaptation: Shifted entirely to remote methods — video interviews and screen-sharing usability tests with patients at home.
Challenge: Diverse patient groups with varying digital literacy, ages, and health complexities. Adaptation: Developed multiple personas and tested each iteration with representatives from each segment.
Challenge: Balancing clinical credibility with community engagement features. Adaptation: Separated clinical tools from community features in the information architecture whilst maintaining visual cohesion.
Challenge: Meeting NHS compliance whilst maintaining agile velocity. Adaptation: Embedded NHS stakeholders in sprint reviews and created compliance documentation in parallel with design.
Approach
1. Remote Stakeholder & Patient Interviews
~15–20 participants · Patients, providers, NHS stakeholders
Remote interviews via video call exploring care disruption, digital adoption barriers, and remote clinical support requirements.
Key findings: Patients felt isolated without in-person appointments. Both patients and providers needed NHS-branded platforms, not third-party apps.
2. Patient & Provider Personas
4 personas · Research-validated
Personas representing patient segments (newly diagnosed, long-term diabetic, digitally confident/cautious) and provider roles (diabetes nurse, GP).
Key findings: Digital literacy varied widely. Community support valued but had to feel clinically safe. Providers needed at-a-glance progress dashboards.
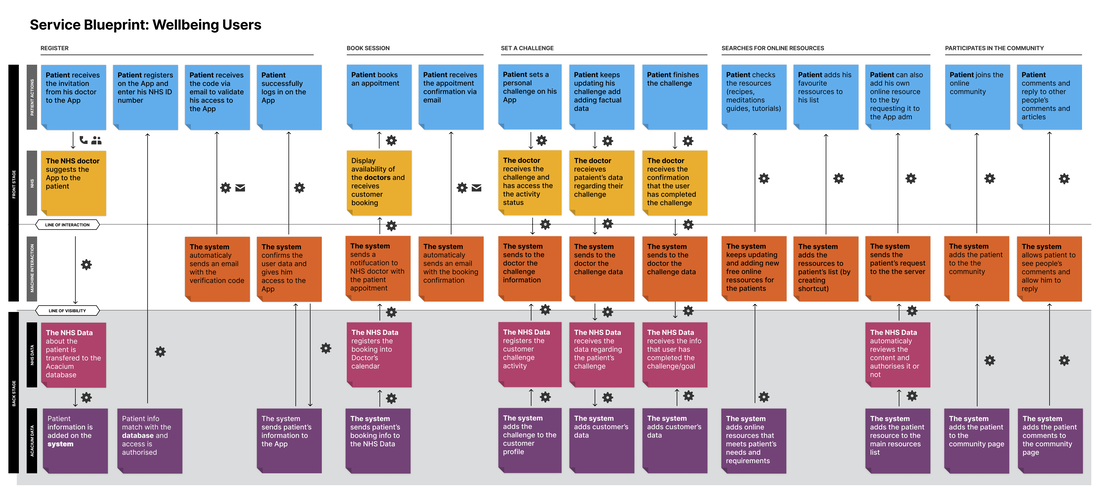
3. Digital Healthcare Journey Mapping
Co-created with patients and providers
Mapped the end-to-end journey identifying touchpoints suitable for digital intervention versus where clinical contact remained essential.
Key findings: Goal-setting, tracking, recipes, and peer support were highly suitable for digitalisation. Virtual consultations needed video and secure messaging.
4. Agile Design Sprints with User Testing
Multiple 2-week sprints · Remote usability testing
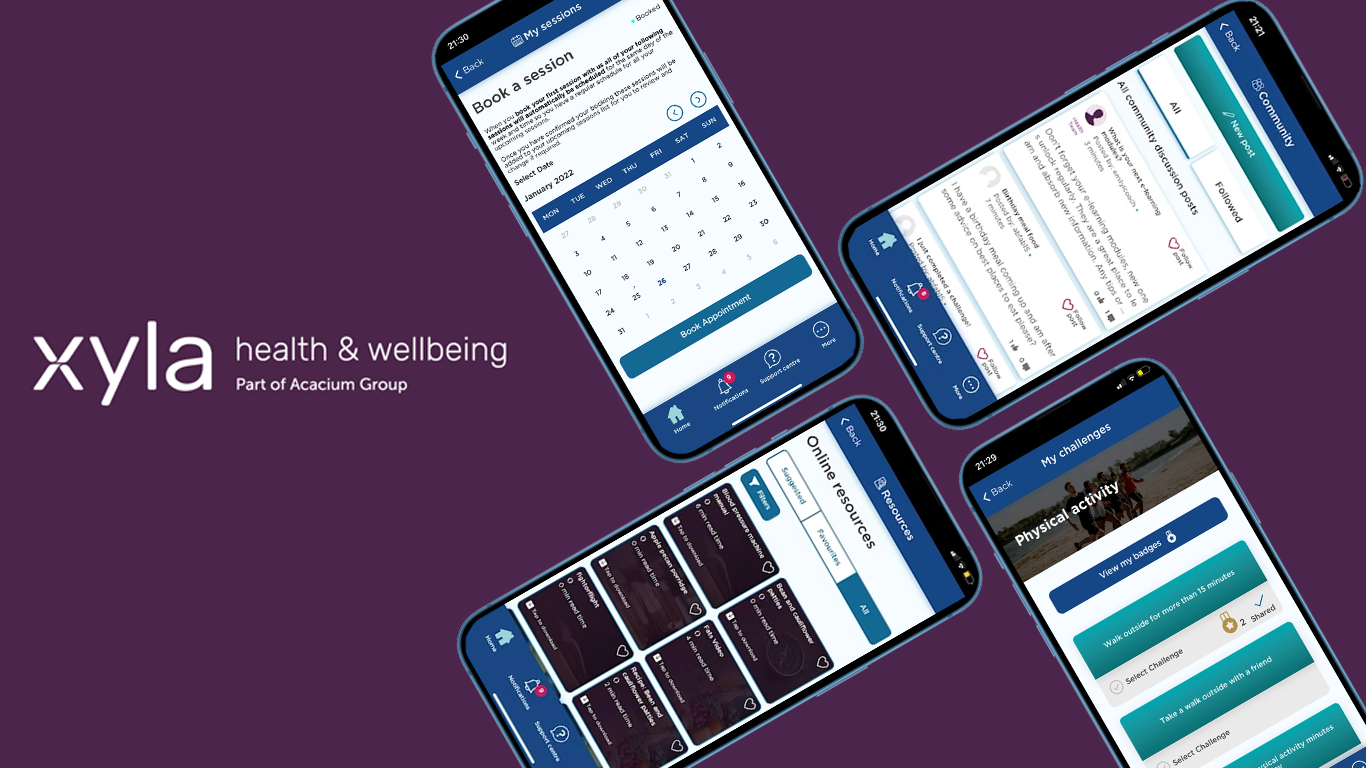
Each sprint delivered a testable feature (consultation booking, forum, recipe database, dashboard). Remote testing via screen-sharing focused on task completion and accessibility.
Key findings: Clear onboarding essential. Forums needed visible moderation. Recipe filtering by dietary requirements critical. Progress visualisations motivated engagement.
5. Clinical Integration & Compliance Review
NHS stakeholders embedded in sprints
Regular reviews with NHS compliance and clinical leads to validate against healthcare standards and data protection requirements.
Key findings: Role-based data visibility required. Community posts needed moderation workflows. NHS branding essential for trust.

Critical findings
RQ1 — How do patients manage without in-person support? Patients felt isolated and turned to unverified online sources, highlighting the need for a trusted NHS digital platform.
RQ2 — Where can digital intervention provide the most impact? Goal-setting, tracking, educational content, and peer support were highly suitable. Virtual consultations could replace routine check-ins but not acute decisions.
RQ3 — What barriers exist to telehealth adoption? Digital literacy varied widely. Patients needed clear onboarding, simple navigation, and NHS-approved reassurance.
RQ4 — How can community support be integrated safely? Community features had to feel moderated and clinically safe to prevent misinformation.
RQ5 — What do providers need? Dashboards showing engagement, progress trends, and flagged concerns. Secure messaging to reduce phone triage workload.
Deliverables
- Patient and provider personas (4 total)
- Digital healthcare journey maps
- Community support framework and moderation guidelines
- Responsive health platform (web and in-app)
- Patient engagement analytics dashboard
- NHS compliance documentation
Impact
- Diabetic patients maintained continuity of care during COVID-19 lockdown.
- Platform launched nationally for NHS service users.
- Community forum reduced patient isolation during pandemic.
- Remote monitoring dashboards reduced clinician triage workload.
- Platform accessible across diverse digital literacy levels.